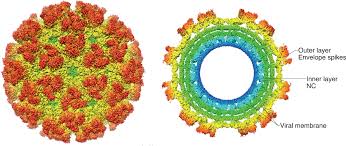
Chikungunya virus (CHIKV) is a mosquito-borne pathogen that has been identified in more than 110 countries around the world. The virus typically causes flu-like symptoms, but it can also trigger chronic, severe joint pain in some people.
Researchers at La Jolla Institute for Immunology (LJI) are working to understand how a viral infection can cause persistent joint pain that closely resembles rheumatoid arthritis, an autoimmune disease.
In a new study, LJI scientists share a critical first look at how the body’s T cells target CHIKV. Their research suggests CD4+ T cells step up to fight the virus — and cause chronic inflammation in the process. This discovery may help explain why some people infected with CHIKV develop severe joint pain.
“Autoimmune diseases like rheumatoid arthritis have exactly these parameters,” says LJI Assistant Professor Daniela Weiskopf, senior author of the new study and member of LJI’s Center for Vaccine Innovation.
The findings, published recently in Cell Reports Medicine, offer new clues to why some viral infections appear to trigger autoimmune disease. The research may also help guide the development of therapies to block harmful inflammation.
Testing immune cells vs. Chikungunya virus
Weiskopf and her colleagues studied immune cells found in blood samples from a group of CHIKV patients in Colombia. The researchers tested how immune cells from these patients responded to small molecular chains, called peptides, from Chikungunya virus.
This experiment revealed which types of immune cells take the lead in fighting CHIKV infection. The researchers also captured the first-ever look at which sites on CHIKV, called viral epitopes, drew the strongest immune cell responses.
To their surprise, the researchers found that a type of T cells called CD4+ T cells showed a strong response to CHIKV. Although CD4+ T cells are a normal part of the body’s anti-viral response, they are almost always accompanied by CD8+ T cells. Scientists have even nicknamed CD8+ T cells “killer” T cells because they play a very active role in fighting infections.
Yet the new study shows that CD4+ T cells are most active in fighting CHIKV virus. These same CD4+ T cells stay in the body as “memory” T cells after the infection is gone.
The researchers found that 87 percent of patients had detectable levels of CHIKV-specific memory CD4+ T cells in their blood six years after their initial infection. In contrast, only 13 percent of patients still had CHIKV-specific memory CD8+ T cells in their blood after six years.
According to Weiskopf, this kind of CD4+ T cell profile is more commonly seen in patients with autoimmune diseases. “I’m an infectious disease researcher, but I could see that this T-cell response looked awfully like what we see in autoimmune disease,” says Weiskopf.